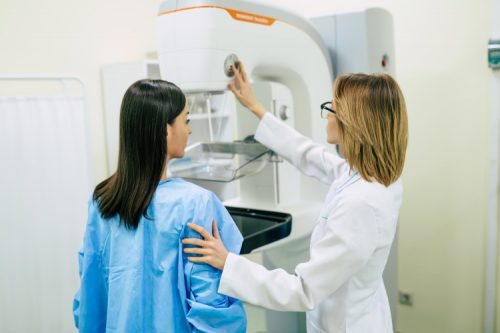
 What do vaccines, handwashing, and routine cancer screenings have in common? All are preventative measures against disease. Preventative care involves intervening before an illness or injury occurs, keeping individuals, families, and populations healthier for longer than they would be without this care.
What do vaccines, handwashing, and routine cancer screenings have in common? All are preventative measures against disease. Preventative care involves intervening before an illness or injury occurs, keeping individuals, families, and populations healthier for longer than they would be without this care.
What is preventative care, and how do health care professionals contribute to prevention? Preventative care can take many forms and address any determinant of health — from providing clean drinking water to mass vaccination programs that eliminate diseases such as smallpox. Nationwide prevention strategies have spared millions of Americans from environmentally-caused diseases, including lead poisoning and lung cancer.
In addition to these measures, continued improvements in health education can support a healthier population. By offering education and counseling both in person and via telehealth services and health apps, nurses play a prominent role in preventative health efforts nationwide.
What Is Preventative Care?
The treatment and management of existing medical conditions is just one aspect of health care. A nurse’s care responsibilities may also include educating patients about strategies for altering risky behaviors (such as smoking and poor eating habits) and conducting screenings to identify diseases before the onset of more serious symptoms.
Examples of Preventative Care
Preventative care measures aim to uncover illness in its early stages — looking for signs that may indicate elevated risk for certain conditions — or protect patients from disease by other means. Some nurse-administered examples of preventative care include the following:
- Cancer screenings. Nurses may screen for certain types of cancer, such as colon and breast cancer, as these diseases are typically far easier to treat if discovered in their earliest stages.
- Annual checkups. During an annual checkup, a nurse may help a patient understand the implications of test results. For example, a nurse may explain the importance of testing a patient’s blood to check for high cholesterol or blood pressure, which can foreshadow heart disease.
- Childhood and adult immunizations. Nurses educate patients about the importance of getting immunized against diseases. Nurses can also help families navigate immunization schedules for their children.
- Annual flu shot. Some pathogens, including the virus that causes the flu, mutate quickly, so annual immunizations are required to provide protection. Nurses can administer the yearly flu shot to prevent illness in individuals and communities
- COVID-19 booster shots. Nurses may also administer COVID-19 vaccines, including a patient’s primary series or booster, which provide temporary defense against serious complications due to the coronavirus.
Timing Preventive Care
Nurses implement preventative measures in accordance with demographic variables like age, gender, and family history. For example, colorectal cancer is widely screened for, but only in adults over 45, according to the Centers for Disease Control and Prevention (CDC). The CDC recommends this age threshold because younger adults are at a much lower risk statistically for this type of cancer.
What Is Health Promotion?
Health promotion is another component of preventative health care. According to the World Health Organization (WHO), health promotion is the practice of educating and encouraging individuals to take greater control of and improve their health. One way to do this is by empowering individuals to effectively manage any chronic conditions that they may have and to take lifestyle steps to reduce the risk of illness.
Approaches to health promotion include the following:
- Addressing risk factors that contribute to poor health outcomes, such as environmental pollutants (unsafe drinking water, unclean air), unhealthy habits (poor diet), and genetic dispositions to disease (such as a history of breast cancer). Nurses address risk factors by educating patients and communities about ways to avoid risk, including monitoring their health through routine screenings, as well as providing tips on nutrition and exercise.
- Addressing symptoms that reduce the quality of life for patients. Nurses can do this through the early detection and treatment of symptoms and by teaching patients how to maintain a healthy lifestyle or rehabilitate.
- Addressing mental health disorders such as depression and anxiety. The WHO reports that 1 in 8 people globally live with a mental disorder. Nurses can empower individuals to manage these conditions through self-care activities and holistic approaches to health care.
Why Is Preventative Care Important?
Preventative health care strategies are introduced to minimize the risk of disease and keep the population as healthy as possible. A majority of the deaths recorded in the U.S. each year — about 6 in 10 — are caused by chronic conditions that are largely preventable, according to 2022 data from the CDC.
In addition to helping curtail disease, preventative health measures help reduce health care costs and the burden on vital services. The U.S. incurs $4.1 trillion in annual health care costs, according to the CDC, and chronic diseases such as heart disease, diabetes, and cancer are the leading drivers of these costs.
Preventative care can also help strengthen the economy and keep people active in society. Preventable chronic illnesses can limit people’s ability to work; conditions such as obesity, high blood pressure, and asthma are particularly costly to the economy in terms of lost work time. Preventative health care is also an effective way to help seniors maintain their health as they age — a period when the risk of chronic conditions increases. This is why preventative habits are important.
Why Are Nurses Important for Preventative Care Efforts?
What is preventative care without nurses? Nursing staff can help advance preventative health care in numerous ways. Below are some of the most impactful strategies.
1. Providing Health Information
According to the American Nurses Association, in addition to duties such as taking vital signs, administering medication, making physical assessments, and delivering test results, nurses play a significant role in disseminating important health information.
Nurses are qualified to talk to patients about a range of health-related topics, from nutrition and exercise to other forms of disease prevention, such as practicing safe sex and refraining from drugs and excessive alcohol use. Education can be delivered in many ways and in many contexts. Nursing professionals may choose to host informational sessions about particular topics, or they may pass on written materials to patients, such as brochures and links to online resources.
Nurses can use patient visits as an opportunity to initiate preventative health discussions. If a patient comes in with joint pain, a nurse can discuss how excess weight can exacerbate pain before introducing weight management strategies. If a young patient seeks medical assistance with a chronic cough, a nurse can seize the moment to initiate a conversation about smoking cessation. Nursing staff can essentially promote health information and wellness strategies whenever they meet patients, helping disseminate important health information in the wider community.
2. Identifying At-Risk Patients
A crucial component of any preventative health care strategy is paying particular attention to the demographics of patients with a high risk for certain diseases. At-risk patients need tailored information about strategies for better health as well as screenings to catch illness and disease early.
For example, patients with a family history of heart disease should be encouraged to receive routine cholesterol and blood pressure testing, and nurses should offer advice about how exercise and good nutrition can help support heart health. Older adults are another demographic that tends to need more preventative health guidance, as they’re at a statistically higher risk for a range of chronic conditions, including diabetes, stroke, and osteoporosis.
3. Facilitating Access to Care
Patients are often uncertain about the kinds of services they’re entitled to under their health plans. Consequently, many miss out on vital preventative services, such as cancer screenings, blood testing, and immunizations. Nurses can counsel patients on the details of their health plans and help connect them with the services they need and are entitled to.
4. Educating the Community
Nursing professionals can partner with local organizations, such as community centers or faith-based groups, to hold events pertaining to public health: a lecture on good nutrition, a blood drive, or a free cancer screening event. In this way, the nurse’s role can extend beyond a medical practice and into the community at large.
With the expansion of telehealth, digital health applications (apps), and wearable technologies like smartwatches that monitor heart rate, nurses also have the opportunity to educate the general public about how to use technology to prevent illness and injury.
Digital Health Apps and Preventive Care
According to Statista, the Google Play Store alone had 54,603 health care and medical apps available in August 2022. When used effectively, these apps can be a crucial component of a preventative care strategy.
The benefits of digital health apps range from providing general support and instruction to helping people with a chronic illness or disease be more accountable for their well-being. The apps also provide an opportunity for ongoing health monitoring outside of a clinical setting by storing important patient health data and sharing medical information with clinical personnel. With health apps, nurses can use the vast array of digital options available to monitor exercise, track vitals, log symptoms, and provide support for a specific disease.
Nurses can use the plethora of apps to connect with patients and provide ongoing assistance, even after an appointment is over. Nurses can also use the data stored within these apps to inform treatment plans. Steering patients toward apps that track symptoms, manage medications, send out appointment reminders, and more can help them stay on top of an illness or a lifestyle challenge that they’re trying to overcome once they leave the clinic.
Offering individuals options that teach them to make healthy decisions while holding them accountable for their choices — as most apps do — can assist them in making positive changes in their day-to-day habits. Using apps in this way can enable patients to take charge of their well-being. Below are some examples of helpful digital health apps.
Fitness Tracking
Whether fitness tracking is done with a built-in tracker on a smartphone or with a downloaded app, users of some form of exercise tracker are more likely to exercise during their leisure time than individuals who don’t use any digital assistance, according to 2022 findings published in The Lancet. This technology can help individuals understand the most effective ways to exercise and stay organized as they build better, healthier habits.
The most popular fitness apps usually integrate a smartphone and a wearable device, like an Apple Watch or FitBit. The apps include features such as distance and pace tracking (especially useful for runners), calorie counters, time on exercise, step counters, and weight tracking. Most apps also monitor sleep patterns and heart rate, give users daily or weekly progress reports, and let individuals compete with other users. To supplement the features of wearable technology, downloading an app that includes preloaded workout routines can motivate individuals by improving the stats on their worn device.
Additional apps that track fitness and wellness data can greatly assist patients during a clinical appointment. By tracking symptoms and medications and taking notes of any specific issues to discuss during an appointment, patients can get the most out of each visit. Patients can provide their nurse practitioner with complete information regarding the condition that brought them to the appointment in the first place, potentially improving the level of treatment they receive.
Condition Monitoring
For patients with a medical condition that requires monitoring, apps that target certain illnesses and diseases can make care and maintenance easier. By allowing users to store essential information related to their condition in a digital format, everything they need goes with them to each medical visit. The apps allow them to present a complete picture of their health to their nurse practitioner or doctor, enabling their provider to develop a proper long-term care plan and implement any necessary treatment changes.
Common medical conditions that have an app directly targeted to them include the following:
- More than 37.3 million Americans had diabetes in 2022, according to the CDC, with another 96 million diagnosed with prediabetes. The app Glucose Buddy monitors glucose levels and tracks carbohydrate intake and exercise to keep patients functioning within healthy blood sugar levels.
- Attention-deficit/hyperactivity disorder. For the millions of people diagnosed with some form of ADHD, the app ADHD Organizer offers support by increasing their productivity through goal setting and daily activity tracking. The app also helps them address areas of behavior that require improvement.
- Lyme disease. Around 300,000 people are diagnosed with Lyme disease each year, according to the CDC. The app iLog Lyme records symptoms, medications, and medication dosages to help evaluate whether the current treatment being administered is the best for the patient. Tracked information can be sent directly to a care provider, and access to a Facebook support group is part of the iLog Lyme package.
Preventative Nursing in a Digitally Connected World
What is preventative care? It’s clear that many activities and procedures fall under the umbrella of preventative care — and that nurses are crucial to communicating and implementing many preventative health measures.
Empowering patients to take preventative measures to support healthy habits and monitor their health builds disease-resilient communities. Through education, screenings, and monitoring, nurses can help patients take charge of their health and make the necessary changes to lead healthier lives.
Nurse managers can help ensure that nursing professionals provide the best possible health education to patients. If you’re eager to climb the career ladder and lead a dedicated team of nurses, consider applying to Bradley University’s Doctor of Nursing Practice program, which offers a Leadership track. Designed to help you study at a time that complements your professional schedule, all coursework can be completed online with practicums you can set up and complete locally.
Recommended Readings
Self-Care for Nurses: Why It Matters
Clinical Nurse Specialist vs. Nurse Practitioner: What’s the Difference?
Certification vs. Licensure for Nurses: What Are the Differences?
Sources:
Centers for Disease Control and Prevention, About Chronic Diseases
Centers for Disease Control and Prevention, Colorectal Cancer Screening Tests
Centers for Disease Control and Prevention, Immunization Schedules
HealthCare.gov, Preventive Care Benefits for Adults
The Lancet, “Effectiveness of Wearable Activity Trackers to Increase Physical Activity and Improve Health: A Systematic Review of Systematic Reviews and Meta-Analyses”
U.S. Department of Health & Human Services, Preventive Care
U.S. Preventive Services Task Force, Recommendations
World Health Organization, Health Promotion
World Research Foundation, Preventative Health Care Helps Everyone
